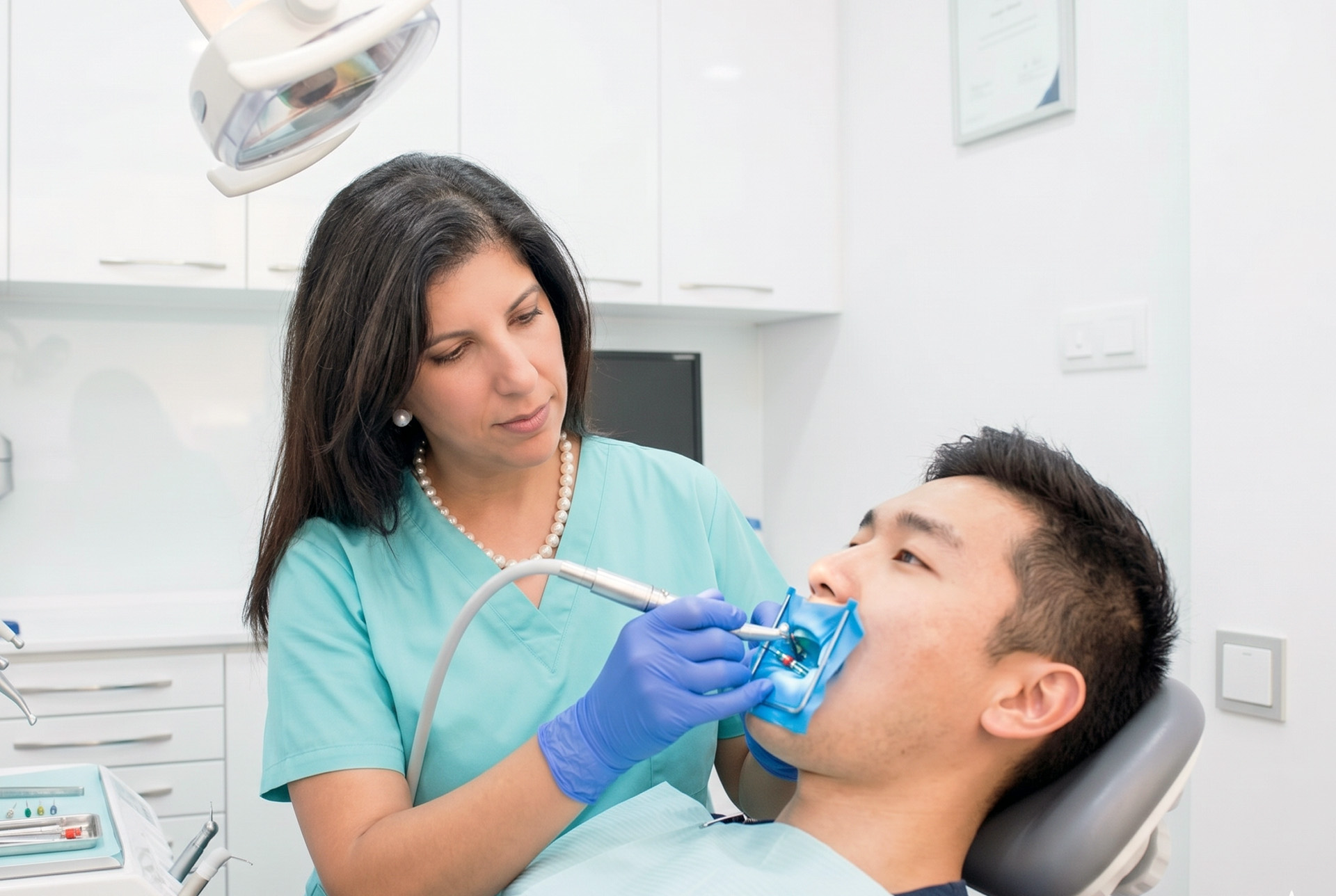
What Is a Failed Root Canal?
Root canal treatment is designed to remove an infection from inside the tooth, clean the root canals, and seal them so the tooth can stay in place and function normally. In many cases, it works very well for years. Sometimes a treated tooth becomes painful, swollen, or diseased again months or even years later, which means the previously treated tooth did not heal properly or became infected again after treatment.
Teeth can have very complex root canal systems, including narrow, curved, or hidden canals that are difficult to clean completely. A failed root canal does not always mean the initial treatment was done badly. Root canal failure can happen even when the original procedure was performed carefully.
Sometimes, root canal failure develops later because new bacteria re-enter the tooth through decay, a leaking filling, a broken dental crown, or a fracture. Salivary contamination is one of the most common causes of root canal failure after the initial treatment. These are the many reasons why it is hard to answer the question, “Why do root canals fail?”, without a specialist taking a careful look at your specific condition.
What are the Symptoms of a Failed Root Canal?
Failed root canal symptoms and side effects often include pain, swelling, pressure on biting, or signs of a new infection around the treated tooth.
The clearest failed root canal symptoms and common signs are persistent root canal tooth pain, pain when chewing, tenderness to pressure, gum swelling, or a pimple-like bump on the gum that may drain pus. Some people also notice an unpleasant taste, persistent bad breath, or sensitivity around the tooth. If the infection has spread further, there may be facial swelling, jaw discomfort, or a fever.
Not every failed root canal causes severe pain. Some cases are picked up because the tooth feels ‘not quite right’, shows tooth discolouration, or becomes tender from time to time. Failed root canal crown symptoms can also appear if the dental crown or filling on top of the tooth becomes loose, cracked or leaky, allowing bacteria to re-enter the tooth. A treated tooth may also fracture, especially if it has lost significant tooth structure or if the final dental crown placement was delayed.
Other symptoms can range from subtle discomfort to obvious swelling or discharge. Some may develop a clear failed root canal infection with swelling or abscess, while others have subtle discomfort that slowly worsens over time.

When to See a Dentist
You should see a dentist if a previously treated tooth becomes painful again, swollen, loose, or tender when you bite down on it.
Mild soreness soon after a root canal treatment can be normal, but tooth pain that persists, returns after a symptom-free period, or is accompanied by swelling, discharge, or a bad taste should be evaluated by a dentist. Early intervention gives the best chance of saving the natural tooth through root canal retreatment rather than extraction.
Urgent review is especially important if you have facial swelling, a fever, difficulty chewing, or a gum abscess near the tooth. These warning signs can point to a failed root canal infection rather than a simple post-treatment sensitivity. Prompt treatment can prevent serious complications such as the spread of infection to other teeth or surrounding structures. Early intervention can make the difference between straightforward retreatment and a more complex medical procedure later on.
Why Do Root Canals Fail?
Root canals fail when bacteria remain inside the tooth, re-enter later, or the tooth develops a new structural problem after treatment.
Some teeth have more canals than expected, unusual branches, or very curved spaces that are hard to detect and disinfect fully. When a dentist misses one of these canals during the original treatment, incomplete cleaning can leave bacteria behind.
Another common reason is leakage from the top of the tooth. If the dental crown placement is delayed, or the crown is loose, cracked, or broken, salivary contamination can recontaminate the inside of the tooth. Salivary contamination through a temporary filling or cracked tooth is a particularly common route for a second infection to develop. This is why a good dental crown is such an important part of root canal success.
The tooth itself can also fracture after treatment. A root canal-treated tooth often begins with a deep decay, large restorations, or structural damage, so it may already be weakened. Vertical root fractures can be especially difficult because they may cause persistent infection even if they initially present with only limited symptoms. Traumatic dental injuries can also contribute to root canal failure by creating cracks or weakening the tooth structure. In some of these cases, saving the natural tooth may not be realistic.
Diagnosis
Diagnosis starts with the patient’s history. Your root canal specialist will ask when the tooth started hurting again and whether the pain is constant or only when biting. They will also examine for swelling, discharge, or a loose crown. The tooth, gum tissue, and bite are then inspected to determine whether the issue is a persistent infection, a cracked tooth, a leak, or something unrelated, such as gum disease or a neighbouring tooth.
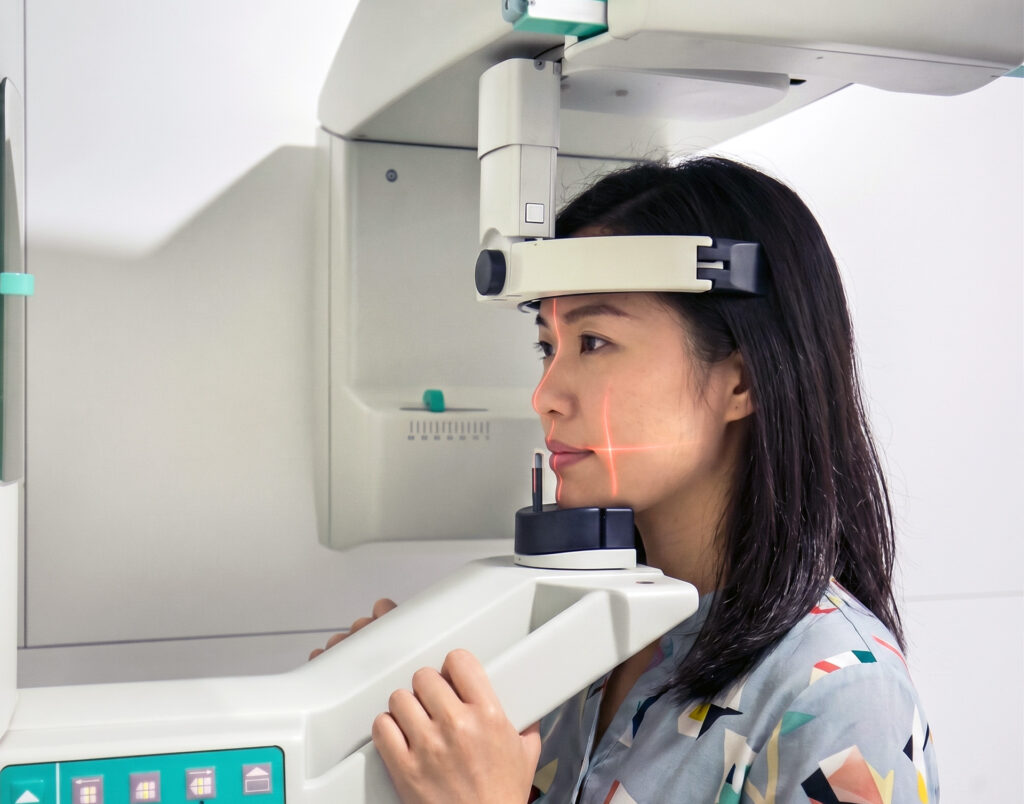
A failed root canal X-ray is often a key part of the assessment. Standard periapical dental X-rays remain the first-line imaging method in endodontics and help the dentist assess root canal structure, filling material, root anatomy, and the bone around the root tip.
An X-ray may show a persistent dark area around the root tip, changes in the supporting bone, or concerns about the existing filling material, although dental X-ray findings are interpreted together with symptoms and examination results. In more complex cases, cone-beam computed tomography may be used because it provides three-dimensional details when conventional X-rays do not clearly answer the question.
Treatment
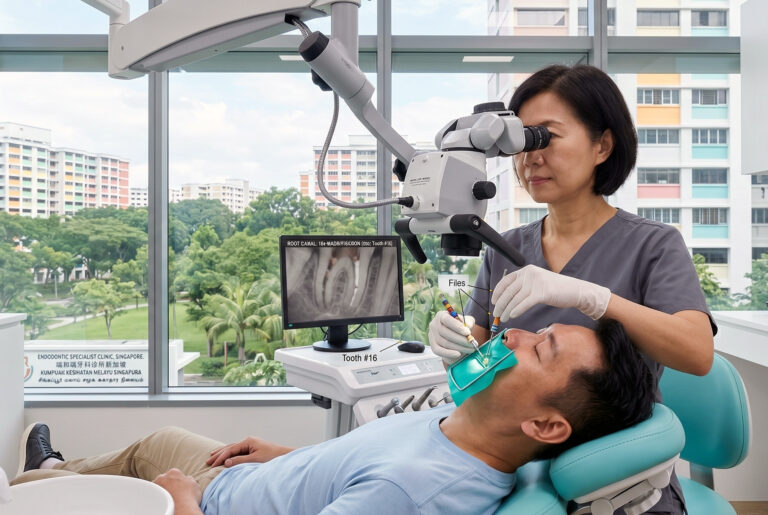
The most common treatment option is nonsurgical root canal retreatment. This endodontic treatment approach involves accessing the tooth, removing the old filling material, cleaning and disinfecting the canals again, carefully looking for missed root canal structure or residual infection, and sealing the canals once more. In many cases, parts of the old restoration, post, or dental crown must be removed first to gain access.
If root canal retreatment from inside the tooth is not enough, endodontic surgery may be considered. This often means apical surgery, in which the root tip is accessed through the gum tissue so the infected area can be cleaned and sealed off from the end of the root. Surgery is more likely to be discussed when canals are blocked, unusually narrow, or otherwise difficult to manage from above. Root canal therapy in the form of surgical intervention can be effective when non-surgical treatment options have been exhausted.
Root canal tooth extraction after a failed root canal is not the first choice, but it becomes the main option when the tooth is too badly cracked, too weak to restore, or not predictable to save. A failed root canal procedure left untreated can lead to serious complications, making proper care essential. Failed root canal extraction is sometimes necessary, especially with a vertical root fracture or extensive tooth structure loss. In these cases, the next discussion is usually about replacement treatment options such as an implant, bridge, or denture.
Risks and Recovery
Recovery depends on the chosen treatment, but early care and good oral hygiene generally improve the chances of healing and preserving the natural tooth.
After root canal retreatment or surgery, some discomfort when biting and mild soreness in the area can be expected for a short period. Your dentist will advise you on pain relief, chewing precautions, and follow-up. Regular check-ups after treatment are important for monitoring oral health and confirming that the affected tooth is healing as expected.
As with any medical procedure, there are no guarantees. Some teeth respond well and function for many years after a root canal retreatment. Others may continue to cause trouble due to complex anatomy, extensive cracks, or severe structural damage. The longer a failed root canal infection is left untreated, the more bone and tooth structure may be lost, and the greater the risk of serious complications affecting other teeth and oral health.
How TEETH @ Tiong Bahru Can Help
TEETH @ Tiong Bahru can help by confirming why the tooth is failing, clearly explaining your treatment options, and aiming to preserve the natural tooth whenever it is sensible and possible.
At TEETH @ Tiong Bahru, assessment focuses on the whole picture: your symptoms, the condition of the restoration, the bite, and what dental X-rays and imaging show around the tooth and its root canals. From there, we can discuss whether the best next step is monitoring, root canal retreatment, referral for more advanced endodontic care, or extraction after a failed root canal if necessary.
Just as importantly, preventing root canal failure from recurring matters. A well-sealed dental crown, good oral hygiene, and regular check-ups all help reduce the risk of bacteria re-entering a root canal-treated tooth. When a failed root canal is recognised early and managed with prompt treatment and proper care, many teeth still have a realistic second chance.
Contact us at TEETH @ Tiong Bahru to schedule a root canal appointment or speak with one of our highly trained dental professionals.
RELATED ROOT CANAL